Nobody wants to hear the words “you need a root canal” — but ignoring the warning signs of a tooth infection can lead to far worse problems, including tooth loss, spreading infection, and even hospitalization. The good news? Modern root canal treatment is comfortable, effective, and saves your natural tooth.
Knowing the signs early gives you the best chance of saving your tooth with the least invasive treatment. Here are 5 warning signs that you may need a root canal — and what to do about them.
What Is a Root Canal?
Before we dive into the signs, let’s quickly clarify what a root canal actually is. Inside every tooth, beneath the hard enamel and dentin, is a soft tissue called the dental pulp. The pulp contains nerves, blood vessels, and connective tissue that helped your tooth develop.
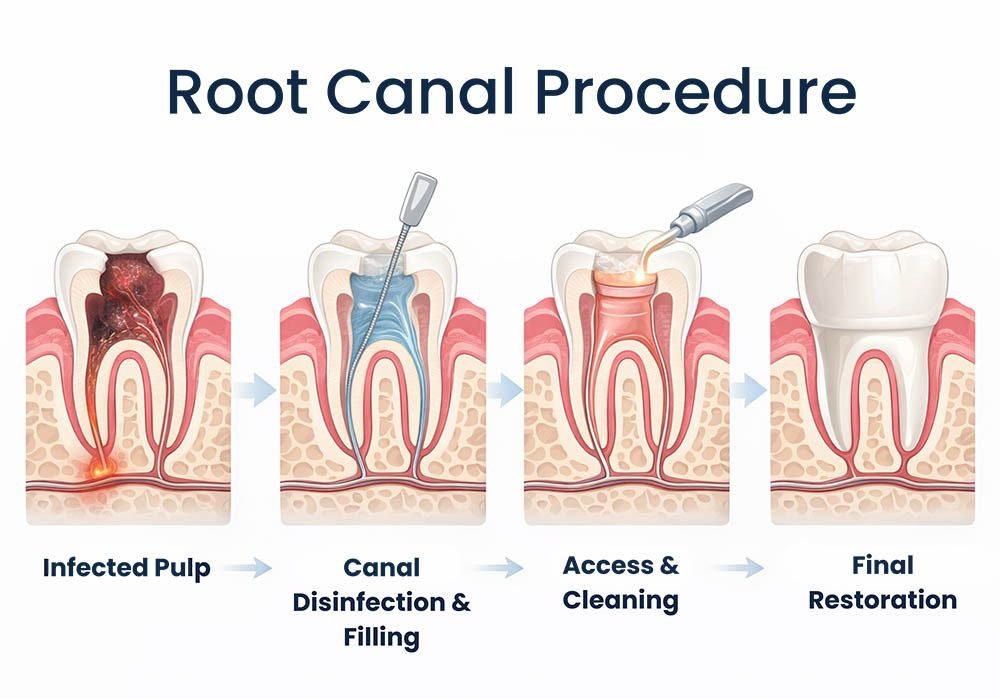
When the pulp becomes infected or inflamed — usually from deep decay, a crack in the tooth, or trauma — it needs to be removed to save the tooth. During a root canal (also called endodontic therapy), your dentist:
- Numbs the area with local anesthesia
- Creates a small opening in the crown of the tooth
- Removes the infected or damaged pulp
- Cleans, disinfects, and shapes the root canals
- Fills the canals with a biocompatible material
- Seals the tooth and places a dental crown for protection
The result? Your natural tooth is saved, the infection is eliminated, and you can eat and smile normally again.
Sign #1: Persistent Tooth Pain
Tooth pain is the most common — and often the most obvious — sign that something is wrong inside your tooth. But not all tooth pain means you need a root canal. Here’s what to watch for:
- Deep, throbbing pain that seems to come from inside the tooth, not the surface
- Pain that wakes you up at night or gets worse when you lie down
- Pain that doesn’t go away with over-the-counter medication
- Pain that radiates to your jaw, ear, or temple
- Spontaneous pain that occurs without any trigger
If your tooth pain is constant, worsening, or disrupting your daily life, it’s time to see a dentist. Persistent pain often indicates that the nerve inside the tooth is inflamed or dying.
What Causes the Pain?
When bacteria enter the pulp chamber through a deep cavity or crack, the pulp tissue becomes inflamed (pulpitis). In the early stages (reversible pulpitis), the inflammation may resolve with treatment. But once the pulp is severely damaged or infected (irreversible pulpitis), the only way to save the tooth is with a root canal.
Sign #2: Prolonged Sensitivity to Hot and Cold
It’s normal for teeth to feel brief sensitivity when eating ice cream or drinking hot coffee. But if the sensitivity lingers for 30 seconds or more after the hot or cold stimulus is removed, that’s a warning sign.
- Normal sensitivity: Brief twinge that disappears in a few seconds
- Concerning sensitivity: Sharp pain that lingers for 30+ seconds after eating or drinking something hot or cold
- Serious sensitivity: Intense pain from hot foods that is relieved by cold — this often indicates the nerve is dying
Prolonged temperature sensitivity usually means the nerve inside the tooth is damaged and struggling to recover. Pay special attention if heat triggers pain but cold provides relief — this is a classic sign of an irreversible pulp problem.
Sign #3: Swollen or Tender Gums
Inflammation near a specific tooth is another telltale sign of infection. Look for:
- Swelling in the gum tissue around one particular tooth
- A small bump or pimple on the gums (called a fistula or parulis) — this is a drainage point for infection
- Tenderness when you press on the gum near the tooth
- A bad taste in your mouth from pus draining through the fistula
Gum swelling associated with a tooth infection is different from gum disease. With an infected tooth, the swelling is typically localized to one area and may come and go. If you notice a “gum boil” or pimple on your gums, don’t pop it — see your dentist right away.
When Swelling Becomes an Emergency
If facial swelling spreads beyond the immediate area of the tooth — especially if it affects your eye, neck, or ability to swallow or breathe — seek immediate medical attention. A spreading dental infection can become life-threatening.
Sign #4: Tooth Discoloration
A tooth that is darkening or turning gray, brown, or black compared to the surrounding teeth may have a dying or dead nerve inside. This discoloration happens because:
- The blood supply to the tooth has been compromised
- The breakdown of internal tissue causes pigmentation changes
- Trauma to the tooth (even years ago) damaged the nerve
Discoloration doesn’t always mean pain — some teeth with dead nerves are completely painless until an infection develops. If one of your teeth is changing color, it’s worth getting it evaluated even if it doesn’t hurt.
A root canal can remove the dead tissue and prevent infection. After the root canal, the tooth can be restored with a dental crown that matches your natural tooth color.
Sign #5: Pain When Chewing or Touching the Tooth
If biting down on a tooth causes pain, or if the tooth is sensitive to touch or pressure, the nerve may be inflamed or the bone around the root tip may be infected.
- Sharp pain when biting on a specific tooth
- Pain when pressing on the tooth with your finger
- Feeling that the tooth sits “higher” than the others (the infection is pushing it upward)
- Pain when tapping on the tooth — your dentist will test this during your exam
This type of pain indicates that the infection has likely spread beyond the tooth root into the surrounding bone. A root canal removes the infected tissue and allows the bone to heal.
What Happens If You Ignore These Signs?
Delaying treatment when you need a root canal can have serious consequences:
- The infection spreads: A tooth abscess can spread to the jaw, neck, or brain, requiring hospitalization and IV antibiotics
- You lose the tooth: A tooth that could have been saved with a root canal may become unsaveable, requiring extraction
- More expensive treatment: An extraction followed by a dental implant costs significantly more than a root canal and crown
- Bone loss: Chronic infection can destroy the bone around the tooth, making future implant placement more complex
- Systemic health risks: Dental infections have been linked to heart disease, diabetes complications, and other systemic health problems
The bottom line: the sooner you get treatment, the better the outcome and the lower the cost.
Does a Root Canal Hurt?
This is the #1 question patients ask — and the answer may surprise you. Modern root canals are no more uncomfortable than getting a filling.
Thanks to advanced anesthesia techniques, flexible nickel-titanium instruments, and digital imaging, root canal treatment today is:
- Virtually painless during the procedure (you’ll be completely numb)
- Faster than ever — most root canals are completed in a single visit lasting 60–90 minutes
- Comfortable — sedation options are available for anxious patients
In fact, the pain you’re experiencing before the root canal is far worse than anything you’ll feel during or after the procedure. Most patients report immediate relief once the infected pulp is removed.
Root Canal vs. Extraction: Which Is Better?
When possible, saving your natural tooth with a root canal is almost always the better choice. Here’s why:
- Cost: A root canal + crown ($1,500–$3,000) costs less than an extraction + implant ($2,449)
- Time: A root canal is completed in 1–2 visits; an implant takes 4–6 months
- Function: Nothing functions as well as your natural tooth
- Bone preservation: Your natural tooth root maintains jawbone stimulation
- Longevity: A properly treated tooth can last a lifetime
Extraction is recommended when the tooth is too damaged to save — severely cracked below the gum line, has extensive bone loss, or has failed a previous root canal that can’t be retreated.
Frequently Asked Questions
How do I know if I need a root canal or just a filling?
If the decay or damage is limited to the outer layers of the tooth (enamel and dentin), a filling is sufficient. If bacteria have reached the pulp (nerve) inside the tooth, a root canal is necessary. Your dentist will use X-rays and clinical tests to determine which treatment you need.
How long does a root canal take?
Most root canals are completed in a single appointment lasting 60–90 minutes. Molars with multiple canals may take slightly longer. In some cases, a second visit may be needed to place the permanent crown.
Can a tooth that needs a root canal heal on its own?
No. Once the dental pulp is infected or severely inflamed, it cannot heal on its own. Antibiotics may temporarily reduce symptoms, but they cannot eliminate the infection inside the tooth. Without a root canal, the infection will continue to spread.
What does recovery after a root canal look like?
Most patients experience mild soreness for 2–3 days after the procedure, easily managed with over-the-counter pain medication. You can return to normal activities the same day. Avoid chewing on the treated tooth until your permanent crown is placed.
How much does a root canal cost?
Root canal treatment typically costs $799 depending on the tooth (front teeth are less expensive than molars). A dental crown is usually recommended after the root canal, adding $799. Most dental insurance plans cover root canals as a major procedure at 50–80%.
Think You Might Need a Root Canal?
If you’re experiencing any of the signs described above, don’t wait for the pain to become unbearable. Early treatment gives you the best chance of saving your tooth comfortably and affordably. At Madison Square Dental in Arlington, TX, our experienced team provides gentle, efficient root canal treatment using the latest techniques and technology.
Or call us at (817) 275-2229 to schedule your evaluation.